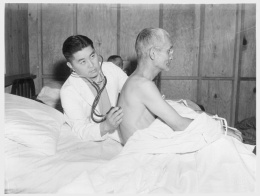
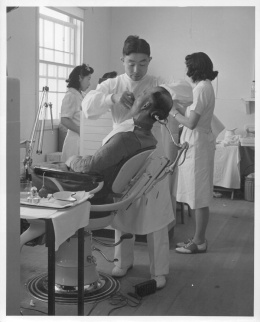
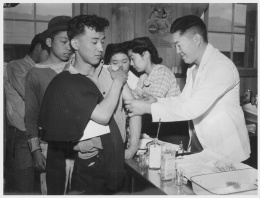
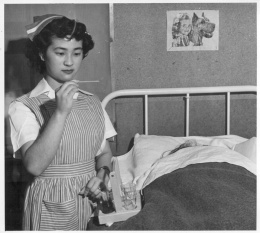
Medical care in camp
At 6:40 a.m. on September 22, 1942, Mrs. Thomas Takaki gave birth to a baby girl while prone atop a dining hall table at the temporary Topaz Infirmary located in the laundry Hall of Block 4. The swaddled infant, nestled into an orange crate bassinet, was named Eugenia, after Dr. Eugenia Fujita, the young attending physician. The infirmary was eleven days older than its first newborn.
Most Nikkei patients encountered similar spartan medical conditions throughout the transition period into incarceration, first in the assembly centers and during the first months of life in the WRA 's so-called "relocation centers."
Prewar Nikkei Health Professionals
Prior to the outbreak of war with Japan, 87 licensed Nikkei physicians and surgeons were practicing medicine in the four western states, 90 percent of them having received their primary medical training in the United States. Other Nikkei health providers included 137 trained nurses, 105 dentists, 132 pharmacists, 35 optometrists, and 92 laboratory technicians and assistants. Most prewar practitioners worked in urban areas where professional opportunities abounded. The Nikkei community in Los Angeles enjoyed a favorable 1:777 physician-to-population ratio (30:23,321); further north, the ratio was 1:480 (11:5,280) in San Francisco. Nikkei city residents could almost always find a physician with similar cultural affinities. Rural communities, comprising half of the total west coast Japanese population, enjoyed fewer options, having to rely more upon Caucasian physicians or traditional folk or herbal medicines, or to forego nonemergency care altogether.
With the coming of Executive Order 9066 and the eviction of communities from the military exclusion zones , beginning in April 1942 Nikkei practitioners were forced to close down their offices. Interns and residents lost hospital positions, and nurses their jobs. A new health care work environment soon awaited them–infirmaries and hospitals located behind barbed wire fences, accompanied by demeaning salaries of less than $20 per month.
Planning the Health Care Program
Executive Order 9066 authorized the Secretary of War to employ any federal agency he believed essential in carrying out the provisions of the president's order, including those of medical and hospitalization. Thus, design and supervision responsibilities fell to the United States Public Health Service (USPHS), with help from state, county, and city health departments. In June 1942 USPHS provided technical guidance for setting up the hospitals and producing the public health standards eventually employed universally.
WRA regulations resulting from planning seminars required an adequate program of health services that embraced both curative and preventive medicine, including all specialized fields, as well as selected fields such as dentistry, nutrition, sanitation, pharmacy, optometry, laboratory services, hospital and public health nursing, midwifery and nurses aides, medical social work, psychiatric social work, and health education services.
USPHS advisers recommended that one physician be made available for every 1,000 inmates, and one nurse for every 200. Even a physician-to-population ratio of 1 to 1,500 would prove unattainable because of the increasing drain on medical manpower caused by the war and because too few Nikkei physicians and nurses were available to meet the demand. More, turnover in Caucasian staff at WRA hospitals was high because of spartan living conditions and the challenges of getting along with the Nikkei staff. Recruitment proved difficult because the WRA had to compete with hospitals and clinics throughout the country begging for help to replace staff going off to war and willing to pay higher salaries and provide comfortable working conditions.
Manpower shortages would later increase when the WRA implemented a resettlement program that enabled physicians, nurses, and other health workers to leave the centers to pursue their careers outside the military exclusion zones.
Health Care in the WCCA Assembly Centers
The army's general policy regarding the health of the Nikkei population under its jurisdiction in the temporary "assembly centers" administered by the Wartime Civil Control Administration (WCCA) was to safeguard the health of the well, prevent spread of communicable disease, care for the sick, and protect the sick and aged at each stage of the incarceration. The USPHS was called upon to provide personnel and consultation and public hospitals to augment the professional services of Nikkei doctors and nurses.
An Issei physician was appointed to oversee all health related activities in each camp and answered to the camp administrator and USPHS advisors. This supervision included managing hospital personnel and setting up and equipping the infirmaries. Because the sojourn in the WCCA centers was intended to last no more than two months, plans called for establishing infirmaries and first aid stations, rather than hospitals. At most locations this meant maternity and surgical cases would be outsourced to public hospitals.
The hastily planned and erected WCCA centers—crowded, unhealthy, unsanitary, and demoralizing, posed strong threats to the public health of the inmates. As a result, the primary activities of the medical staffs centered on an inoculation program against typhoid fever, diphtheria, smallpox, and whooping cough. Medical staffs immunized thousands of inductees thereby causing significant delays in preparations to open most infirmaries for general care. At Manzanar , during a three month period beginning March 22, 1942, the resident medical staff administered 28,923 typhoid inoculations and 11,475 smallpox immunizations.
Unsanitary conditions resulted in outbreaks of food poisoning at many of the WCCA centers due to lack of proper storage equipment and inexperienced food handlers. A severe outbreak of diarrhea at the Puyallup Assembly Center caused by spoiled Vienna sausages nearly caused a panic among sentries in the guard towers. Symptoms started at night after everyone was in bed. Public latrines were located some distance away from most barracks, and the lighting along the roads was poor or nonexistent; thus, people took flashlights to light their way. Finding one set of stalls occupied some scurried to another, and pinpoints of light appeared like fireflies in the dark. The sentries, momentarily fearing an insurrection, threw on the spotlights and called for reinforcements. Order was quickly restored, and the epidemic passed without major incident.
Once the inoculation program ended, obstetrical, general medical, and minor outpatient surgical care consumed most of the time and energies of the resident medical staff. The maternity program proved to be a highlight during the early incarceration period, which carried over into the WRA camp experience. A total of 504 live births were recorded during the seven month period. Prenatal care was universal. Most mothers were referred to nearby county public hospitals for birthing, but immediately returned to camp to complete the customary two-week recovery period on the maternity ward. All centers provided well-baby care, offering clinical and home visits. And during transfers to the WRA centers mothers with infants received preferential Pullman accommodations, as well as prepared formulas and special food and supplies of diapers.
Health Care in the WRA Centers
The transition to health care for Nikkei in the WRA centers proved as challenging as the WCCA center experience. In many instances new inductees found their new place of incarceration not prepared to receive them. Instead of fully operational hospitals, patients and medical staffs were greeted with rudimentary first aid stations and infirmaries. Despite a relatively long planning and construction period, for the first several months center hospitals and infirmaries proved under designed, under equipped, under supplied, and under staffed. Basic supplies were limited, with essential equipment often missing, such as sterilizing equipment, which made surgical care impossible.
At Gila River construction on the hospital building was not completed until four months after the center opened. Essential x-ray equipment had not arrived. No ambulances were available for the 640 acre compound. At Poston three months passed before basic supplies reached the hospital. In the meantime, essential medications were difficult if not impossible to obtain.
Compounding the problems at the WRA centers, all authority enjoyed by the senior Nikkei physicians at the WCCA centers was stripped away and given to Caucasian male physicians brought in as medical directors; Caucasian female chief nurses usurped the authority of both Nikkei nurses and physicians. Thus, inductee medical workers had little authority to effect policy, staffing, or how health operations were to be run.
This demotion in status led to morale and staffing problems that were never fully resolved. At Heart Mountain , the lack of cultural competency and poor judgment on the part of the Caucasian chief medical officer allowed professional jealousies and rivalries among the stressed Nikkei physicians to get out of hand. This, combined with resentments built up against the Caucasian authority led to the staff turning on each other resulting in two hospital walkouts in 1943 that put the camp population at risk. Similar resentments led to incidents at Poston and Manzanar.
However, despite personal humiliations associated with being forcefully removed from civilian life, low wages, and ongoing contentious relations with their Caucasian counterparts, the Nikkei medical staffs helped build a health care system that offered universal health care to all who were incarcerated. This occurred in the presence of overworking, understaffing, living in poor housing with little privacy, and enduring harsh environments with extreme temperatures in summer and winter. In one case, at Poston Dr. Hashiba urged the windows in surgery be sealed to prevent swirling dust from the outside seeping in through the tiniest cracks.
Hospitals at Full Capacity
In time, each WRA center fulfilled its mission to operate a full service inpatient and outpatient hospital. From May 1942 until March 1946 when the last center, Tule Lake , closed, the hospitals recorded a total of 5,981 live births and 1,862 deaths, and countless inpatient and outpatient services.
At Topaz , 3,973 hospital admissions were recorded during its 36-month life, a per month average of 110 inpatients. Admissions reached a high of 181 in April 1943. Nikkei physicians performed 29 surgeries that month, 18 of them appendectomies. Outpatient visits averaged 1,886 per month, with seasonal fluctuations. In December 1943, for example, the infirmary was overwhelmed with patients from an influenza epidemic sweeping the country. Officials reported 1,100 cases at Topaz, alone, and school absenteeism exceed 25 percent during the two-week siege. Although these numbers were significant, other centers fared worse.
Dental Care
While the shortage of medical personnel proved endemic, this problem did not carry over to the dentists, who were overrepresented at most centers and less likely than their physician counterparts to leave for resettlement. Hospital dental clinics operated closer to full capacity and for longer and uninterrupted periods than the various medical wards.
The dentists had their own problems, however, that centered on the lack of equipment and supplies. Many had at their disposal only what they brought with them from their prewar practices. More than one dentist hired a carpenter to modify a straight-back wood chair to produce a working dental chair, which would remain in use until arrival of equipment retrieved from storage.
Dental care consisted primarily of basic fillings, extractions, and denture fabrication. At Topaz, the hospital dental clinic handled an average of 1,365 patient visits per month, which peaked at 1,899 visits in April 1943. In addition, the clinic participated in a nationwide epidemiological survey of children sponsored by the National Institutes of Health to determine the causes of tooth decay. In July 1943 the staff examined nearly 1,400 resident school aged children, representing 75 percent of the eligible children.
Medical Staff Shortages Increase
The WRA's expanding resettlement policy enabled hospital staff to resume normal professional lives outside the exclusion zones. These departures produced severe hospital staff shortages. Most who resettled were Nisei who possessed the energy to relocate and reestablish themselves, representing those with the greatest eagerness to regain their freedom. Dr. Paul Suzuki, a prewar Seattle physician incarcerated at Minidoka , was conflicted between serving his incarcerated Seattle community or resettling to provide a more healthy environment for his wife and infant. He chose to enter a practice in Spokane, outside the exclusion zone, as a steppingstone to returning to Seattle after the war.
Issei health professionals saw less opportunity on the outside and many of the older cadre elected to stay behind. At Poston, by spring of 1943 only the four Issei physicians remained. Replacements of the Nisei doctors were Caucasian.
To help alleviate staff shortages a core of nurses' aides, in their late teens and 20s were trained. Soon hospital staffs came to rely on them. For example, at Poston, in 1944 75 Nisei nurses aides assisted 14 graduate nurses. Despite the manpower shortages, the 70 Issei women who had listed their profession as midwives, were not permitted to be used as childbirth attendants. Since the hospital was considered the center of camp health services, all babies were delivered by physicians. Instead they were used as public health assistants, providing prenatal and postnatal care in home visits and well-baby clinics.
Ongoing Health Risks
Unlike the WCCA centers that were located within or nearby large concentrations of Nikkei populations, the WRA centers were set up in arid desert and high plains regions, with extreme temperatures in the summer and winter, and in swamplands with serious drainage problems. These adverse environmental conditions may have contributed to health problems of the imprisoned populace, especially the two most vulnerable groups, the very young and very old.
Dust was ubiquitous in the high desert locations. At Amache , residents experienced dust storms three or four times a month for eight months out of the year. At Gila River and Poston, coccidioidomycosis, with its influenza and pneumonia-like symptoms, was endemic and put most inmates at risk. Inmates living in the swirling dust environments also suffered increased rates of asthma. At the Arkansas camps malaria remained a public health threat until the mosquito hazard was brought under control in mid-1943.
As in the WCCA centers the food supply was also a source of illness, arising as a result of unsanitary food handling practices, lack of proper equipment, and inadequate refrigeration. Acute food poisoning from salmonella occurred in 199 reported cases at Minidoka during the first three months of operation. Such problems were soon brought under control, but minor epidemics of diarrhea continued throughout the life of the centers.
Crowded conditions elevated the threat of tuberculosis. The disease accounted for 11 percent (206 cases) of the 1,862 deaths recorded. Vigilant public health efforts implemented to prevent its spread likely prevented more fatalities.
The most frequent causes of death were cancer of all types (407), heart disease (293), tuberculosis (206), vascular disease (197), pneumonia/influenza (70), and kidney disease (70).
Conclusion
The WRA and USPHS undertook an enormous task to provide acceptable health care for more than 100,000 people incarcerated in unfriendly physical environments in World War II. Poor administrative planning and coordination, inadequate human and physical resources and the frailties of human beings living under the strain of imprisonment conspired to compromise the government's goal to provide universal access to health care in the camps.
Despite this, an entire population received inoculations against debilitating or potentially fatal diseases. Expectant mothers had access to prenatal and postnatal preventive care, which many prewar mothers had never enjoyed for lack of availability of the service or ability to pay for it. And for some, the definitive dental care in the centers was the first such experience in a lifetime.
Certainly many cases of medical misfortunate befell Japanese Americans during their incarceration. Many camp survivors providing testimony at the 1981 Commission on Wartime Relocation and Internment of Civilians (CWRIC) hearings cited a lack of proper health care for themselves and their families. The belief that poor health care outcomes were a direct result of expulsion from their prewar homes remains strong to this day.
Worth remembering, however, is that by the end of the war one third of active physicians throughout the country had left their communities to serve in the armed forces. If not incarcerated, Japanese Americans would have been affected by the declining physician pool since at least sixty of the 87 prewar, practicing Nikkei physicians were of draft-eligible age. And with all west coast cities filled with war production workers, Nikkei residents would necessarily have had to compete with the expanding population for available health resources.
That the health care system worked as well as it did is a testament to the dedication and fortitude of Nikkei health workings toiling under difficult circumstances and to the resiliency of the Japanese American people themselves who made the best of a wartime situation over which they had little control.
For More Information
Fiset, Louis. "Health Care at the Central Utah (Topaz) Relocation Center," Journal of the West 38(2) (1999): 34-43.
———. "Public Health in World War II Assembly Centers for Japanese Americans," Bulletin of the History of Medicine 73 (1999): 565-584.
———. "The Heart Mountain Hospital Strike of June 24, 1943." In Remembering Heart Mountain: Essays on Japanese American Internment in Wyoming , edited by Mike Mackey. Powell, WY: Western History Publications, 1998.
Hirahara, Naomi, and Gwenn M. Jensen. Silent Scars of Healing Hands: Oral Histories of Japanese American Doctors in World War II Detention Camps . Michi Nishiura and Walter Weglyn Multicultural Publication Series, 2004.
Jensen, Gwenn M. "System Failure: Health-Care Deficiencies in the World War II Japanese American Detention Centers," Bulletin of the History of Medicine 73 (1999): 602-628.
U.S. Department of the Interior. The Evacuated People: A Quantitative Description . Washington, D.C.: Government Printing Office, 1946.
Last updated Aug. 29, 2024, 2:06 p.m..

 Media
Media